Raffi Balian sits in his office at the South Riverdale Community Health Centre and casually recalls the day he saved his former girlfriend’s life after she overdosed on Fentanyl, a drug that is more potent than morphine.
His ex-girlfriend actually overdosed “three times in the same day,” says Balian. Each time was from using Fentanyl, a synthetic analgesic narcotic.
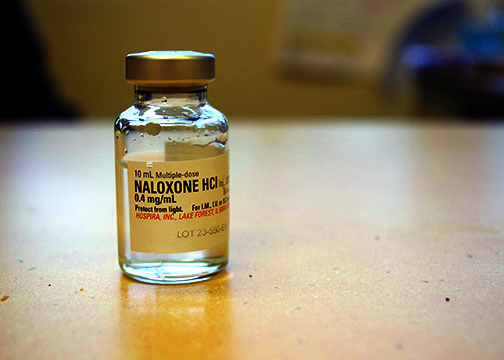
Balian credits a so-called “miracle drug,” officially known as Naloxone, for her survival.
The federal government recently released statistics citing a 40 per cent rise in opiate overdoses since 2004. A shocking number for most, but not for Balian, who coordinates the Counterfit Harm Reduction program, which aids in safer drug use at the South Riverdale Community Health Centre.
“We were the ones who flagged that overdose was going to increase in the city,” he said.
“We anticipated this when Oxycontin was banned. When Oxycontin went out of the market there was a big niche,” he said of the banned prescription painkiller.
“People started to buy heroin but there wasn’t enough … so they found ways to synthesize Fentanyl, and because Fentanyl is so much stronger, people are taking too big of a dose.”
To give you an idea of its potency, the opiate Fentanyl is up to 20 times stronger than street-level heroin, gram-to-gram.
Balian himself has been injecting opiates, including heroin and Fentanyl, for the past 22 years. It is all too easy to underestimate the strength of new drugs and how to use them, says Balian. Sometimes fatal errors are made.

Raffi Balian is coordinator of the Counterfit Harm Reduction program at the South Riverdale Community Health Centre.
This is where Naloxone comes in. The opiate may be a user’s best friend. Balian explains how the drug works and why it’s so important to put it in the hands of every opiate user.
“Nalaxone is a drug that blocks the opiate receptors, so if someone is overdosing and you inject Naloxone … in a few minutes these take over the receptors that bind to opiates,” Balian says. “The person who is overdosing all of a sudden wakes-up. It’s like a miracle drug.”
The Works, a harm reduction organization run by the City of Toronto, distributes Naloxone through its Point program. The group hands out kits, which includes two doses of Nalaxone.
However, one main issue with the distribution of Naloxone is that it’s only useful if there is someone there to administer it.
Shaun Hopkins, manager of the Works needle exchange program, says getting Nalaxone in the hands of friends and families of opiate users can be challenging.
“Naloxone is prescription medication, so we need to follow a medical directive to provide it,” says Hopkins.
“We have to provide it to the person who is addicted to the opiates, so, what we do is have that person come in with a family member, a friend, someone they use with, so we can train all of them on how to use the kit. At this point though, because this is a prescription medication, we have to give this kit to the person who uses the opiate.”
Since 2011, the Point program has handed out more than 2,000 kits and, according to Hopkins, they have received feedback that they’ve been used successfully in more than 300 overdose situations.
Balian believes there is a need for supervised injection sites, as well as the deregulation of Nalaxone to make it affordable. He says an increase of doctors overseeing needle exchange programs is also essential.
“Deregulating it, making it possible for pharmacists to sell them over the counter, you can’t abuse this [Naloxone],” he says.
Balian says doctors should be obligated to hand out Nalaxone with every opiate prescription.
“It doesn’t do any harm. Doctors have to give them out. They have to be mandated to give them [Nalaxone] out with every opiate prescription … Naloxone has decreased the amount of overdoses amazingly in this area.”

You didn’t mention the 24 people that died in alcohol related auto accidents, or the 13,369 who dies from cigarette smoking, every single day. Your ex overdosed three times in one day from Fentanyl? She obviously needs to be in a mental institution. %40 increase since 2004? I guess you failed to see the Harvard study showing the number of counties with people over 65 had gone up %600 in the last ten years. Older people are far more prone to painful injuries..DUH. Another advertisement disguised as “NEWS”. OPIATE HYSTERIA, the new, if it bleeds, it leads, article, now run every day across the nation. ALL of them failing to mention the real causes of death in America, because the Fed and states get billions of tax dollars from the sale of these killers.